Use the labels in the right column to find what you want. Or you can go thru them one by one, there are only 32,362 posts. Searching is done in the search box in upper left corner. I blog on anything to do with stroke. DO NOT DO ANYTHING SUGGESTED HERE AS I AM NOT MEDICALLY TRAINED, YOUR DOCTOR IS, LISTEN TO THEM. BUT I BET THEY DON'T KNOW HOW TO GET YOU 100% RECOVERED. I DON'T EITHER BUT HAVE PLENTY OF QUESTIONS FOR YOUR DOCTOR TO ANSWER.
What this blog is for:
My blog is not to help survivors recover, it is to have the 10 million yearly stroke survivors light fires underneath their doctors, stroke hospitals and stroke researchers to get stroke solved. 100% recovery. The stroke medical world is completely failing at that goal, they don't even have it as a goal. Shortly after getting out of the hospital and getting NO information on the process or protocols of stroke rehabilitation and recovery I started searching on the internet and found that no other survivor received useful information. This is an attempt to cover all stroke rehabilitation information that should be readily available to survivors so they can talk with informed knowledge to their medical staff. It lays out what needs to be done to get stroke survivors closer to 100% recovery. It's quite disgusting that this information is not available from every stroke association and doctors group.
Saturday, July 26, 2025
Effects of Segmental Muscle Vibration on Flexor and Extensor Groups of the Upper Limb in Enhancing Functional Recovery After Stroke: A Randomized Trial
Monday, December 23, 2024
Upper extremity function and disability recovery with vibration therapy after stroke: a systematic review and meta-analysis of RCTs
Absolutely fucking useless! You didn't write a rehab protocol from all this earlier research, did you?
focal muscle vibration (7 posts to May2020)
vibration (37 posts to February 2011)
Whole Body Vibration Therapy (7 posts to January 2016)
Upper extremity function and disability recovery with vibration therapy after stroke: a systematic review and meta-analysis of RCTs
- Yueh-Hsun Lu,
- Hung-Ju Chen,
- Chun-De Liao,
- Po-Jung Chen,
- Xin-Miao Wang,
- Chieh-Hsiang Yu,
- Po-Yin Chen &
- Chueh-Ho Lin
Journal of NeuroEngineering and Rehabilitation volume 21, Article number: 221 (2024) Cite this article
Abstract
Background
This study aimed to investigate the therapeutic effects of vibration therapy for improving upper extremity motor impairment, function, and disability recovery in people with stroke.
Design
We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analysis guidelines. PubMed, EMBASE, the Cochrane Library Database, Physiotherapy Evidence Database (PEDro), China Knowledge Resource Integrated Database, and Google Scholar were searched from inception to May 31, 2024. Randomized controlled trials (RCTs) that evaluated the effects of vibration therapy on upper extremity motor impairment, function, and disability recovery post-stroke were analyzed.
Setting and participants
Participants with a diagnosis of stroke with hemiplegia (or hemiparesis) were recruited.
Methods
Methodological quality assessment was performed using the PEDro quality score. Upper extremity motor impairment, function, and disability were the primary outcomes. Upper extremity motor impairment was measured using the Fugl-Meyer Assessment scale and other methods. Upper extremity functions were evaluated using the Wolf Motor Function test or other tools assessing manipulative activities. Disability was assessed using the Functional Independence Measure, Barthel index, and other methods.
Results
Overall, 30 RCTs including 1621 people with stroke were selected. Compared with the control, vibration therapy exerted significant effects on upper extremity motor impairment [standardized mean difference (SMD) = 1.19; p < 0.00001)], function (SMD = 0.62; p < 0.00001), and disability recovery (SMD = 1.01; p < 0.00001). The subgroup analysis revealed that focal vibration therapy (SMD = 2.14) had favorable effects on disability recovery compared with whole-body vibration therapy (SMD = 2.0). Interventions lasting 4–8 weeks showed significant improvements in motor impairment (SMD = 1.19), motor function (SMD = 0.57), and disability (SMD = 0.84); additionally, the effects of vibration therapy combined with conventional rehabilitation (SMD = 1.03) were superior to those of vibration therapy alone (SMD = 0.21).
Conclusions
Vibration therapy may be(You aren't familiar with earlier research, are you? YOU'RE FIRED!) a reliable rehabilitation program to improve upper extremity motor functions and disabilities. Furthermore, vibration therapy should be performed at the earliest possibility after stroke for at least 4–8 weeks.
Trial registration The protocol of this study was registered with PROSPERO (Registration number: CRD42022301119).
Background
Brief Summary Vibration therapy (VT) significantly reduces upper extremity (UE) motor impairment, enhances UE motor function, and improves disability outcomes in people with stroke. Combining VT with standard rehabilitation is recommended, starting as early as possible after a stroke and continuing for at least 8 weeks. Both low and high vibration frequencies are effective, but focal muscle vibration is particularly beneficial for disability recovery.
Feeding, dressing, and writing are the most common activities of daily living that require motor function and participation of the upper limbs [1, 2]. These activities are essential for maintaining independence and quality of life. Neurologic disorders such as stroke, which often results in hemiparesis, where one side of the body becomes weak or paralyzed, may lead to poor motor function, muscle weakness, spasticity in paretic limbs, and disability [1, 2].
Full recovery of motor function and disabilities of the upper limbs occurs in less than 20% of people with stroke undergoing rehabilitation programs [1, 3]. Hence, many of these people with stroke have poor motor function and disability in the upper limbs, affecting their quality of life substantially [4, 5]. This impairment often necessitates long-term rehabilitation and support to manage daily activities [2, 3]. Consequently, independence and social participation can be significantly compromised for these individuals.
Compared with previous rehabilitation programs, vibration therapy (VT) stimulates muscle activity through the excitation of the tonic vibration reflex which activates efferent Ia, resulting in α-motor neuron excitation to generate muscle fiber strength and induce motor function performance [6, 7]. This implies that weak muscle activity and motor function in paretic limbs could be improved using VT. Recent studies investigated the effects of the whole-body vibration (WBV) on improving disabilities in the upper limbs for people with stroke by asking them to sit on a chair and place their hands on the WBV platform [8, 9]. After 4 weeks of the intervention, the people with stroke in the experimental group treated with WBV showed better motor function improvements in the upper limbs than those in the control group undergoing a traditional rehabilitation program [8, 9]. Furthermore, several studies have developed focal muscle vibration (FMV) to improve motor function and disabilities in people with stroke [10,11,12].
However, vibration force transmission from WBV or FMV to the targeted upper limbs is different being a complex process that could be influenced by various biomechanical mechanisms and result in different outcomes according to the type of vibration application [13, 14]. Previous studies often used vibrations < 20 Hz for muscle relaxation and reduction of spasticity [15, 16]. Research also shows that vibrations in the range of 20–30 Hz can improve gait balance [17]. Since the resonance frequencies of some important human organs are between 5 and 20 Hz, previous studies have considered 20 Hz as a safety threshold for vibration frequency [18].
Hence, optimal vibration protocols to improve motor function and disabilities should be established with strong evidence before applying them to improve motor and functional recovery in individuals with stroke in the clinical setting [7, 19, 20]. Therefore, it is crucial to develop an optimal evidence-based VT protocol for improving motor function and disability recovery to help clinical therapists enhance upper limb recovery in people with stroke.
Despite the potential of VT, its use in the upper extremities (UEs) and benefits on function and disability recovery have rarely been discussed; furthermore, evidence-based treatment effects are not well-established. Therefore, this meta-analysis aimed to investigate the effects of VT protocols on UE motor impairment, function, and disability recovery in people with stroke.
More at link.
Thursday, March 21, 2024
Promising New Wearable Could Retrain the Brain After Stroke
I got this from amazon when I was around enough to get packages; vibration motor
and I'll put together something like the research shows.
Promising New Wearable Could Retrain the Brain After Stroke
A new and deceptively simple advance in chronic stroke treatment could be a vibrating glove.
Researchers at Stanford University and Georgia Tech have developed a wearable device that straps around the wrist and hand, delivering subtle vibrations (akin to a vibrating cellphone) that may relieve spasticity as well as or better than the standard Botox injections.
"The vibro-tactile stimulation can be used at home, and we're hoping it can be relatively low cost," said senior study author Allison Okamura, PhD, a mechanical engineer at Stanford University, Stanford, California.
For now, the device is available only to clinical trial patients. But the researchers hope to get the glove into — or rather onto — more patients' hands within a few years. A recent grant from the National Science Foundation's Convergence Accelerator program could help pave the way to a commercial product. The team also hopes to expand access in the meantime through larger clinical trials with patients in additional locations.
The work builds on accumulating research exploring vibration and other stimulation therapies as treatments for neurological conditions. Other vibrating gloves have helped reduce involuntary movement for patients with Parkinson's. And the University of Kansas Medical Center, Kansas City, Kansas, will soon trial the Food and Drug Administration-approved vagal nerve stimulator, an implantable device intended to treat motor function in stroke survivors. Okamura noted that devices use "different types of vibration patterns and intensities," depending on the disease state they target.

Spasticity often develops or worsens months after a stroke. By then, patients may have run out of insurance coverage for rehabilitation. And the effectiveness of Botox injections can "wear out over time," Okamura said.
In a clinical trial, patients wore the device for 3 hours a day for 8 weeks, while doing their usual activities. The researchers continued testing their spasticity for 2 more weeks. Symptom relief continued or improved for some patients, even after they stopped using the device. More than half of the participants experienced equal or better results than another group that only received regular Botox injections.
How Vibro-Tactile Stimulation May Rewire the Brain
The device originated at Georgia Tech, where Okamura's postdoctoral research fellow Caitlyn Seim, PhD, was using vibro-tactile stimulation (VTS) to teach people skills, such as playing the piano, using touch-feedback training. The team decided to target spasticity, which VTS had helped in previousstudies of in-clinic (non-wearable) devices.
How does the device work? The researchers point to neuroplasticity, the ability of neurons to create new synapses or strengthen existing ones in the brain.
"The stimulation is sending additional sensory signals to the brain, which helps the brain interpret and reconnect any lost circuits," Okamura said.
Spasticity is driven by "an imbalance in the excitatory drive to the muscles,” she continued. This can lead to worsening contractions, until a hand closes into a fist or a foot curls up. (The team has also done preliminary research on a similar device for foot spasticity, which they hope to continue developing.) Previous studies by Okamura and others suggest that vibration stimulation may prevent these contractions, both in the short and long term.
"Immediately, we do see some softening of the muscles," Okamura said. "But in our longer-term study, where we compared to Botox, I also think that the vibration may be retraining the brain to send inhibitory signals. And that can restore balance that's lost due to the damaged neural circuits from a stroke."
When the team did a separate study comparing the effects of muscle and skin stimulation, they hypothesized that the vibration could be having a biomechanical effect on the muscle. Instead, they found that stimulating the skin had a greater impact — a "somewhat unexpected" result, Okamura said. That led them to the brain.
"Stimulating the skin is really about creating sensory signals that get sent to the brain," Okamura said, "which is why we think it's actually a brain-retraining effect and not a direct biomechanical effect."
What's Next?
The researchers are seeking funding for longer-term clinical studies to find out if effects persist beyond 2 weeks. They also want to explore how long and often patients should wear the glove for best results.
The researchers also want to study how movement might enhance the effects of the device.
"One of the treatments for spasticity — medications aside, this vibration machine aside — is more exercise, more passive range of motion," said Oluwole Awosika, MD, associate professor at the University of Cincinnati College of Medicine, Cincinnati, Ohio, who was not involved in the study. "It would have been nice to have a control group that didn't get any of this stimulation or that was only encouraged to do 3 hours of movement a day. What would the difference be?"
Awosika also wondered how easy it would be for stroke patients without in-home assistance to use the device. "Sometimes wearing these devices requires someone to put it on," he said.
Of course, if all goes well, patients wouldn't have to deal with that forever. "The dream would be that you reach true rehabilitation, which is no longer needing the device," Okamura said.
Thursday, February 22, 2024
Comparison of tendon and muscle belly vibratory stimulation in the treatment of post-stroke upper extremity spasticity: a retrospective observational pilot study
Where is the protocol on this so survivors can train their 'professionals' in it?
Comparison of tendon and muscle belly vibratory stimulation in the treatment of post-stroke upper extremity spasticity: a retrospective observational pilot study
Scientific Reports volume 14, Article number: 4151 (2024) Cite this article
-
17 Altmetric
Abstract
Previous studies have reported the effects of vibratory stimulation (VS) therapy in reducing upper extremity spasticity after stroke. However, the effective location of the VS in patients with stroke remains unclear. This study aimed to determine the VS location that is most effective in reducing post-stroke finger and wrist flexor spasticity. We enrolled 27 consecutive patients with stroke and upper extremity spasticity in this retrospective observational study. The participants received stretching, tendon vibration, and muscle belly vibration for 5 min over a period of 3 days. To evaluate spasticity, we assessed the Modified Ashworth Scale score before and immediately after each treatment and immediately after voluntary finger flexion. Participants who received tendon vibration showed greater improvement in flexor tone in the fingers than participants who received stretching and muscle belly vibration (P < 0.05 and < 0.001, respectively). Participants who underwent VS showed no significant improvement in the wrist flexor tone compared to those who underwent stretching. Our results suggest that the tendon may be the most effective location for treating spasticity of the finger flexor muscles and that VS may not significantly improve spasticity of the wrist flexors more than stretching.
Introduction
Spasticity is a movement disorder characterized by a velocity-dependent increase in muscle tone, with exacerbated tendon reflexes1. Upper extremity spasticity occurs in approximately 35% of patients within 6 months of stroke onset2. Severe spasticity is more common in the upper than in the lower extremities2. Stroke patients may experience joint contractures, muscle pain, and limitations in their daily activities due to spasticity. This spasticity can also become a barrier to improving upper extremity function3,4. This highlights the importance of treating spasticity to facilitate the improvement of upper extremity hemiparesis.
Although botulinum toxin injection5,6,7,8 and intrathecal baclofen therapy9 are well-tolerated and effective treatments for spasticity after stroke, these therapies require special clinical skills and are invasive procedures that may cause pain. Moreover, these therapies are usually not cost-effective10 due to their high cost. In contrast, stretching11, extracorporeal shock wave therapy12,13, neuromuscular electrical stimulation14, and vibratory stimulation (VS)15,16,17 serve as non-pharmacological and non-invasive alternatives for the treatment of spasticity.
The American Heart Association guidelines recommend that VS be considered a non-invasive and effective treatment for reducing spasticity18. Three randomized controlled trials reported that local muscle VS may be a useful tool with anti-spastic effects when applied directly to the spastic muscles of the hemiplegic upper extremity after stroke15,16,17. Of these studies, Noma et al.15 implemented VS on the tendon and Costantino et al.16 implemented VS on the muscle belly; both studies reported improvement in muscle tone as measured by the Modified Ashworth Scale (MAS). However, no previous studies have compared the effects of VS on the muscle belly and tendon on upper extremity spasticity in patients with stroke. Owing to a lack of knowledge, no consensus has been reached as to whether the muscle belly is a more effective location than the tendon in VS therapy for spasticity. A recent systematic review of the effectiveness of VS for spasticity in patients with stroke also suggested that treatment effectiveness may vary depending on the target muscles and the degree of spasticity19.
This study aimed to determine whether VS of the tendon or muscle belly is more effective in reducing spasticity of the finger and wrist flexors in patients following stroke. Investigating the most effective location may enhance the effectiveness of VS therapy for spasticity in patients with stroke.
Methods
Study design and research participants
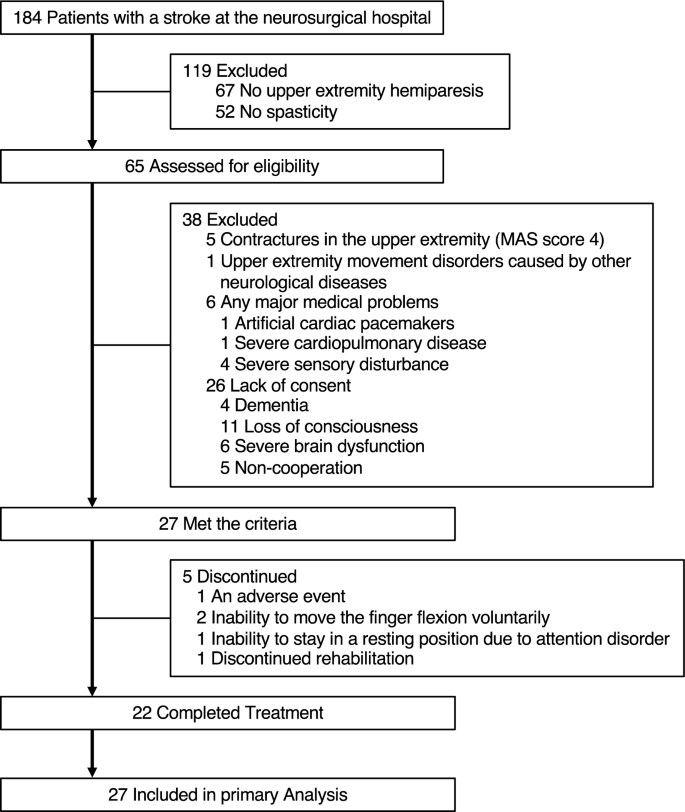
This retrospective observational study was conducted at our hospital. We recruited 27 consecutive patients with stroke who met the following criteria (Fig. 1): upper extremity hemiparesis, abnormal muscle tone of the affected wrist or finger flexors (MAS score 1–3); age > 20 years, and providing informed consent between November 2018 and March 2019.
The exclusion criteria were as follows: contractures in the upper extremity (MAS score 4), upper extremity movement disorders caused by other neurological diseases, and any major medical problems determined by the physician (artificial cardiac pacemakers, severe cardiopulmonary disease, or severe sensory disturbance).
The study was approved by the nonprofit organization MINS Institutional Review Board (acknowledgment number: 180229), and was designed according to the 1975 Declaration of Helsinki, as revised in 1983. The trial was registered in the University Hospital Medical Information Network Clinical Trial Registry (UMIN000043457), which is a public trial registry.
Procedure
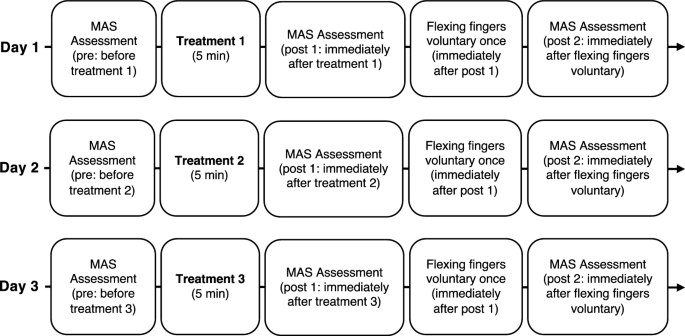
Figure 2 shows the typical procedure. The participants received three treatments once a day for 3 days. The order of treatment was randomized for each participant by the author. Occupational Therapist in charge of patient’s treatment performed the treatments and evaluations. The authors created a manual for the evaluation and treatment procedures based on previous studies15,20. We handed it out to the occupational therapists responsible for the evaluation and treatments. All occupational therapists underwent instruction in the methodology for assessing muscle tone through the Modified Ashworth Scale (MAS) and received training in three distinct therapeutic modalities under the author's guidance during practical skills development. The MAS scores were recorded three times for each treatment: before treatment (pre), immediately after treatment (post 1), and immediately after voluntary finger flexion (post 2).
Study design time flow. The order of the three treatments was randomized for each participant. Three treatments consisted of stretching for the wrist and finger flexor muscles, vibration stimulation therapy on the tendon of the wrist and finger flexor muscles, and vibration stimulation therapy on the muscle belly of the wrist and finger flexor muscles. MAS: Modified Ashworth Scale.
Participants flexed their fingers voluntarily immediately after recording the post 1 MAS scores, which were recorded again (post 2) to assess the lasting effect of reducing spasticity.
This study is not blinded in its evaluation, treatment, or analysis.
Interventions
The participants received the following three treatments: (1) stretching of the wrist and finger flexors, (2) VS therapy for the tendon of the wrist and finger flexors, and (3) VS therapy for the muscle belly of the wrist and finger flexors. The participants received each treatment for 5 min. During each treatment, the participants lay in the supine position and were asked to relax their muscles, as muscle contractions can interfere with the effects of the VS. If they could not receive the interventions in the supine position, they received the treatments in the sitting position.
In each treatment, the participant’s arm was placed in the maximum extension position using a specific device (Fig. 3A) to suppress the initial intense contraction by VS. The device had a movable wrist joint section that could be adjusted to fix the wrist joint in the maximum extension position. The device and treatment methods used were based on a previous study15. The device was developed by Teijin Pharma Ltd, Tokyo, Japan.
The device used to fix the upper extremity and apply vibratory stimulation. (A) The Wrist and finger joints placed in the maximal extension position. (B) Vibratory stimulation on the tendon of the wrist and finger flexor muscles. (C) Vibratory stimulation on the muscle belly.
VS was applied to the tendon or muscle belly of the wrist and finger flexors using a vibration massager with spherical rubber and a vinyl-covered head (diameter: 5 cm) (Thrive MD-01; Thrive Co. Ltd., Osaka, Japan) (Fig. 3B,C). The vibration frequency was set to 91 Hz at an amplitude of 1.0 mm.
Measurement of muscle tone
The MAS20 was used to individually evaluate the spasticity of the wrist and finger flexors, and the scales rated the resistance perceived when moving an extremity passively about a joint in six grades (0, 1, 1+, 2, 3, and 4). A score of 0 indicates normal muscle tone, and 4 indicates rigid flexion or extension. MAS has mainly been used in previous studies to evaluate the spasticity of the biceps brachii, wrist flexors, and finger flexors20. For data analysis, MAS scores (0, 1, 1+, 2, 3, and 4) were assigned numerical values called “calculated MAS scores” (0, 1, 2, 3, 4, and 5, respectively)21.
We placed the joint in a maximally flexed position and moved it to a position of maximal extension for one second20.
The response rate was used to evaluate the response of spasticity to each treatment. This was defined as the proportion of participants with at least a 1-point improvement from baseline (pre) on the MAS.
Statistical analysis
No statistical sample size calculations were conducted. However, we conducted post-hoc power and effect size analyses using the results for the 27 participants in this study in GPower version 3.1. We calculated post-hoc power and effect size from the sum of the squares calculated in the analysis of variance.
This study included data from participants who did not complete the entire study process in the data analysis. Non-parametric statistics were used for the analyses because not all data met the normality criterion. This study did not compare patient characteristics between treatments because the three different treatments were administered to the same subjects. The effects of the interventions over time on the MAS scores were evaluated using 2-way repeated measures analysis of variance (ANOVA) with a post-hoc Bonferroni-corrected Wilcoxon test (number of comparisons = 3). Between-group differences in MAS scores were analyzed using the Kruskal–Wallis test and Bonferroni-corrected Wilcoxon test (number of comparisons = 3). To compare response rates between interventions, McNemar’s test was conducted. The threshold for significance was set at P < 0.05. All statistical analyses were performed using JMP version 17.0 software (SAS Institute Japan, Tokyo, Japan).
Results
Table 1 provides participants’ demographic information. The number of participants included in the analysis for each treatment is shown at the bottom of Figs. 4 and 5. One participant presented with blushing, a hot feeling, and swelling as adverse events after VS of the muscle belly. However, the symptoms improved the following day. Five participants received partial treatment because of an adverse event (N = 1), inability to move the finger flexion voluntarily (N = 2), inability to stay in a resting position due to attention disorder (N = 1), and discontinued rehabilitation (N = 1).
More at link.