Use the labels in the right column to find what you want. Or you can go thru them one by one, there are only 32,720 posts. Searching is done in the search box in upper left corner. I blog on anything to do with stroke. DO NOT DO ANYTHING SUGGESTED HERE AS I AM NOT MEDICALLY TRAINED, YOUR DOCTOR IS, LISTEN TO THEM. BUT I BET THEY DON'T KNOW HOW TO GET YOU 100% RECOVERED. I DON'T EITHER BUT HAVE PLENTY OF QUESTIONS FOR YOUR DOCTOR TO ANSWER.
What this blog is for:
My blog is not to help survivors recover, it is to have the 10 million yearly stroke survivors light fires underneath their doctors, stroke hospitals and stroke researchers to get stroke solved. 100% recovery. The stroke medical world is completely failing at that goal, they don't even have it as a goal. Shortly after getting out of the hospital and getting NO information on the process or protocols of stroke rehabilitation and recovery I started searching on the internet and found that no other survivor received useful information. This is an attempt to cover all stroke rehabilitation information that should be readily available to survivors so they can talk with informed knowledge to their medical staff. It lays out what needs to be done to get stroke survivors closer to 100% recovery. It's quite disgusting that this information is not available from every stroke association and doctors group.
Tuesday, March 31, 2026
Sunday, March 29, 2026
Stroke rehab goes high-tech: UP study reveals robotic therapy may restore lost grip
Come back when you finish the job correctly! Will restore using these EXACT PROTOCOLS! 'May' is not a valid result!
What will you do about those like me that have dead brain there and no longer have any signals coming thru? Do you actually have any brains at all that might be useful in solving stroke to 100% recovery?
Stroke rehab goes high-tech: UP study reveals robotic therapy may restore lost grip
MARCH 29, 2026 — The University of the Philippines has just dropped a study that could change how we look at stroke recovery in the country. Researchers Micah Angelo Bacani and Manuel Ramos Jr. from UP Diliman’s Electrical and Electronics Engineering Institute tested a robotic hand orthosis powered by surface electromyography (sEMG) signals — and achieved an impressive 86% response accuracy rate. In plain language: the device listens to muscle signals from the arm and translates them into movement, giving stroke survivors a shot at regaining control of their grip.
Why does this matter? Stroke remains one of the leading causes of disability in the Philippines. Many survivors struggle with long-term loss of hand function, making everyday tasks — from holding a spoon to signing a document — frustratingly difficult.
Traditional rehab often relies on repetitive, passive exercises. But this study argues that recovery is stronger when patients actively participate, engaging their neurological pathways rather than just following preset motions.
That’s where robotics step in: machines that respond to the patient’s own muscle signals, not just programmed routines.
The researchers explained, “Using surface electromyography (sEMG) signals from the arm, the recovering stroke patient can control the robotic assistive device for rehabilitation. This is the myoelectric hand orthosis.”
Additionally, the study found a direct, proportional relationship between the patient’s intended force and the device’s response. In other words, the harder the patient tries, the stronger the orthosis reacts.
Now, that’s not just science — it’s empowerment. Imagine the psychological boost of seeing your effort instantly translated into movement, instead of waiting months for uncertain progress.
Of course, this raises bigger questions for us. Will our healthcare system embrace robotic rehab, or will it remain locked in academic journals? Can public hospitals afford such technology, or will it be another innovation reserved for private clinics and the wealthy? And most importantly, will patients trust machines to help them heal?This study is a reminder that science is racing ahead, but policy and accessibility often lag behind. If robotics can truly help stroke survivors reclaim their independence, then the challenge is no longer technological — it’s social, economic, and political.
When machines can help us heal, will the Philippines let technology be a lifeline for the many, or a luxury for the few?
Poststroke Fatigue: An Overlooked Barrier to Functional Recovery
Oh for fucks sake; stop writing this crapola and just solve fatigue! Oh, you don't have the brainpower to do that simple task? Then go back to playing in your sandbox and let the adults work at it!
Let's see how long everyone in stroke has been incompetent at this problem!
- post stroke fatigue
(58 posts to January 2018)
At least half of all stroke survivors experience fatigue Known since March 2017
Or is it 70%? Known since March 2015.
Or is it 40%? Known since September 2017.
Poststroke Fatigue: An Overlooked Barrier to Functional Recovery
PSF HINDERS FUNCTIONAL CAPACITY AND RECOVERY AFTER STROKE
WHY PSF REMAINS UNDERPRIORITIZED IN STROKE REHABILITATION?
PROPOSED FEATURE‐BASED FRAMEWORK TO CONCEPTUALIZE PSF

CALL TO ACTION: INTEGRATING PSF INTO STROKE REHABILITATION
CONCLUSIONS
Sources of Funding
Footnotes
Split Protein Builds the Infrastructure for Weight Loss
My doctor obviously knew nothing about weight gain post stroke. He didn't reference body metabolism slowing down after age 50 and my limited exercise ability which I used to do to excess allowing me to eat as I wanted. This incompetence led me to a 30 lb. weight gain which I'm still working to conquer.
Will your competent? doctor and hospital at least get research going that delivers EXACT PROTOCOLs TO INITIATE THIS?
Do you prefer your doctor, hospital and board of director's incompetence NOT KNOWING? OR NOT DOING? Your choice; let them be incompetent or demand action!
Split Protein Builds the Infrastructure for Weight Loss
Summary: While current weight-loss blockbusters like GLP-1s focus on suppressing appetite, researchers have uncovered a completely different strategy: increasing energy expenditure by “building out” the body’s natural heat-generating tissue.
The study reveals how a protein called SLIT3 acts as a “split signal” to grow the essential nerve and blood vessel networks within brown fat. Without this infrastructure, brown fat cannot receive the brain’s “get warm” signals or the nutrients it needs to burn calories. This discovery suggests that obesity could be treated by enhancing the body’s internal “metabolic sink” rather than just eating less.
Key Facts
- The “Split Signal”: When brown fat cells secrete SLIT3, an enzyme called BMP1 cleaves it into two fragments. One fragment grows the blood vessels (supplying fuel), while the other expands the nerves (supplying the “on” switch).
- The Metabolic Sink: Activated brown fat acts as a “sink,” drawing in glucose and lipids from the bloodstream to generate heat (thermogenesis) instead of storing them as white fat.
- The PLXNA1 Receptor: Researchers identified PLXNA1 as the specific docking station for SLIT3 that controls nerve density. Mice lacking this receptor couldn’t maintain their body temperature in the cold because their brown fat lacked the “wiring” to hear the brain’s signals.
- Human Evidence: Analyzing fat samples from over 1,500 people, the team found that SLIT3 gene expression is closely linked to metabolic health, inflammation, and insulin sensitivity in individuals with obesity.
Source: NYU
Researchers have determined how a key protein activates brown fat by expanding blood vessels and nerves in the heat-generating tissue.
The findings, published in Nature Communications, point to a potential strategy for treating obesity that deviates from the current approach of suppressing appetite.
Most of the fat in our bodies is white fat, which stores excess energy and, at too high of levels, can lead to obesity. Humans and other mammals also have a smaller amount of brown fat, a specialized tissue that regulates body temperature and is closely linked to weight loss and metabolic health. When activated by exposure to cold, brown fat uses the body’s resources like glucose and lipids to generate heat, a process called thermogenesis.
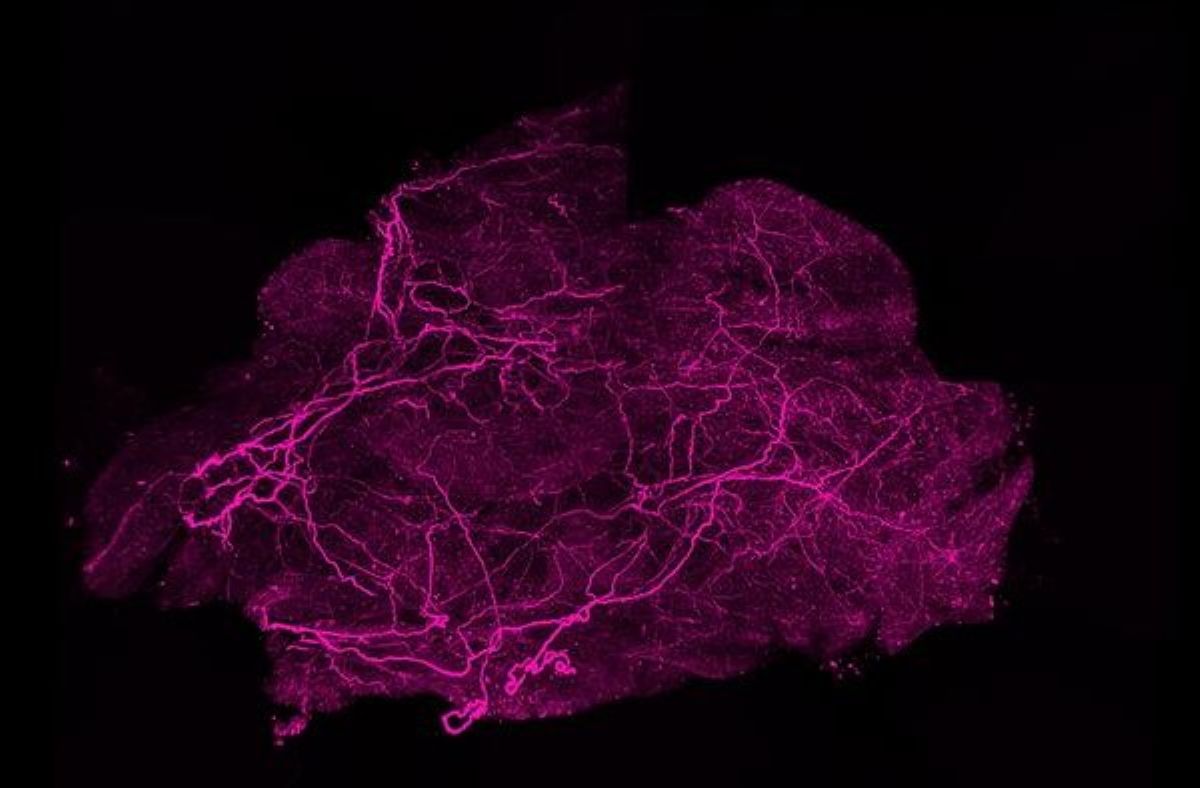
“During thermogenesis, all of that chemical energy is dissipated as heat instead of being stored in the body as white fat,” said Farnaz Shamsi, assistant professor of molecular pathobiology at NYU College of Dentistry and the study’s senior author.
“By rapidly taking up and using fuel sources from our bodies and the food that we eat, brown fat acts like a metabolic sink that draws in nutrients and prevents them from being stored.”
Brown fat has intricate, dense networks of nerves and blood vessels that are critical for its functioning. Nerves enable brown fat to communicate with the brain; when the brain senses cold, it rapidly signals to activate brown fat.
Blood vessels supply brown fat with oxygen and nutrients to generate heat, and then distribute this heat throughout the body. While research on brown fat has largely focused on stimulating fat cells to generate heat, less is known about how these underlying networks function.
Shamsi’s lab previously used single-cell RNA sequencing to identify SLIT3, a protein secreted by brown fat cells, which they thought may play a role in how fat cells communicate. When produced, SLIT3 gets cleaved into two different fragments.
In the Nature Communications study, using a combination of approaches in human and mouse cells, the researchers discovered the enzyme, BMP1, that is responsible for cleaving SLIT3 into two. They also determined that the two SLIT3 fragments control different processes: one grows the network of blood vessels, while the other expands the network of nerves.
“It works as a split signal, which is an elegant evolutionary design in which two components of a single factor independently regulate distinct processes that must be tightly coordinated in space and time,” noted Shamsi.
In addition, the researchers identified the receptor, PLXNA1, that binds to one of the SLIT3 fragments to control brown fat’s network of nerves. In studies in mice—which typically have very active brown fat and can tolerate cold temperatures for long periods of time—removing SLIT3 or the PLXNA1 receptor from brown fat resulted in mice becoming sensitive to cold and having difficulty maintaining their body temperatures. A closer look at brown fat tissue missing SLIT3 or its receptor revealed that it lacks the proper nerve structure and density of blood vessels.
To see if their findings translate to humans, the researchers examined samples of fat tissue from more than 1,5000 people, some of whom had obesity. Focusing on the gene that produces SLIT3, which prior studies show is associated with obesity and insulin resistance, they found that SLIT3 gene expression may regulate fat tissue health, inflammation, and insulin sensitivity in people with obesity.
“That really got our attention, as it suggests that this pathway could be relevant in human obesity and metabolic health,” said Shamsi.
While most weight loss drugs—including GLP-1s—suppress appetite, decreasing the amount of food people eat and therefore the amount of energy stored, treatments that involve brown fat have the potential to increase energy expenditure.
This new understanding of what’s happening inside brown fat—including how SLIT3 splits into two and binds to receptors to control nerves and blood vessels—highlights several processes that could potentially be harnessed for their therapeutic potential.
“Our research shows that just having brown fat isn’t enough—you need the right infrastructure within the tissue for heat production,” said Shamsi.
Additional study authors include Tamires Duarte Afonso Serdan, Heidi Cervantes, Benjamin Frank, Akhil Gargey Iragavarapu, Qiyu Tian, Daniel Hope, and Halil Aydin of NYU College of Dentistry; Chan Hee Choi and Paul Cohen of Rockefeller University; Anne Hoffmann and Matthias Blüher of the University of Leipzig; Adhideb Ghosh and Christian Wolfrum of ETH Zurich; Matthew Greenblatt of Weill Cornell Medical College; and Gary Schwartz of Albert Einstein College of Medicine.
Funding: The research was supported in part by the National Institutes of Health (K01DK125608, R03DK135786, R01DK136724, RC2DK129961, R35GM150942), the G. Harold and Leila Y. Mathers Charitable Foundation, the American Heart Association (24CDA1271852), the Einstein-Mount Sinai Diabetes Center, the NYU Dentistry Department of Molecular Pathobiology, and the Boettcher Foundation.
Key Questions Answered:
A: As senior author Farnaz Shamsi points out, “just having brown fat isn’t enough.” If your brown fat doesn’t have the right “infrastructure”—meaning enough nerves to hear the brain’s signals and enough blood vessels to get oxygen—it stays dormant. It’s like having a high-performance engine with no fuel line or ignition switch.
A: Most current drugs (GLP-1s) work by telling your brain you aren’t hungry, which reduces the energy going in. This SLIT3 pathway is about increasing the energy going out. By “upgrading” your brown fat, you are essentially turning up your body’s internal thermostat to burn through stored white fat and blood sugar.
A: We may not need to grow more brown fat, but rather optimize what we already have. By harnessing the SLIT3-PLXNA1 pathway, scientists hope to develop therapies that “renovate” existing brown fat, making it more efficient at drawing in and burning off excess nutrients.
Editorial Notes:
- This article was edited by a Neuroscience News editor.
- Journal paper reviewed in full.
- Additional context added by our staff.
About this neurology and aging research news
Author: Rachel Harrison
Source: NYU
Contact: Rachel Harrison – NYU
Image: The image is credited to Shamsi Lab, NYU College of Dentistry
Original Research: Open access.
“SLIT3 fragments orchestrate neurovascular expansion and thermogenesis in brown adipose tissue” by Tamires Duarte Afonso Serdan, Heidi Cervantes, Benjamin Frank, Akhil Gargey Iragavarapu, Qiyu Tian, Daniel Hope, Chan Hee J. Choi, Anne Hoffmann, Adhideb Ghosh, Christian Wolfrum, Matthew B. Greenblatt, Paul Cohen, Matthias Blüher, Halil Aydin, Gary J. Schwartz & Farnaz Shamsi. Nature Communications
DOI:10.1038/s41467-026-70310-9