I have seen nothing where stroke medical 'professionals' have anything for oxygen delivery or increased cerebral blood flow post stroke. If you are that concerned; CREATE AN EXACT OXYGEN DELIVERY PROTOCOL!
But nothing will occur, there is NO leadership in stroke directing a stroke recovery strategy to completion! Probably because there is NO strategy!
Hyperoxaemia in acute brain injured patients: too much of a good thing?
The brain is vulnerable to oxygen deprivation because it relies on continuous aerobic metabolism. Even brief interruptions in oxygen delivery lead to rapid ATP depletion, membrane depolarization, excitotoxic neurotransmitter release, and cellular injury. Within minutes, this can progress to irreversible neuronal damage. Accordingly, adequate oxygen delivery is a cornerstone of neurocritical care. However, liberal use of oxygen also has risks because it exposes patients to the potential pathophysiological consequences of hyperoxaemia [1] (Fig. 1).
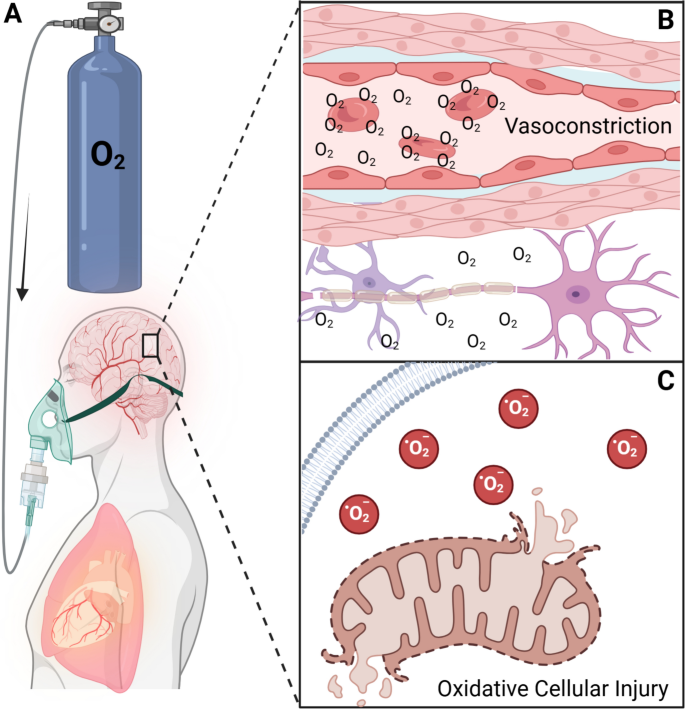
Pathophysiology of hyperoxaemia and its effect on the brain. High fraction of inspired oxygen (A) leads to hyperoxaemia may result in vasoconstriction of cerebral arterioles that can paradoxically reduce oxygen delivery to vulnerable areas of the injured brain where cerebral autoregulation is impaired (B). High arterial oxygen tension increases generation of reactive oxygen species damaging lipids, proteins, and DNA. Mitochondrial injury, both impairs antioxidant defence mechanisms and cellular respiration (C). While oxidative damage to endothelial cells may contribute to disruption of the blood–brain barrier. Endothelial injury may also promote platelet aggregation contributing to microvascular thrombosis and impaired tissue perfusion
Supplemental oxygen therapy is widely available, inexpensive, and readily modifiable at the bedside. Unlike brain tissue oxygenation-focussed strategies (e.g. brain tissue oxygen monitoring [PbtO₂], jugular venous saturation, or near-infrared spectroscopy), titration of inspired oxygen can be applied globally, including in resource-limited settings (despite even basic pulse oximetry and reliable medical oxygen supplies are not universally available in all global health contexts). Given the enormous global burden of morbidity and mortality associated with acute brain injuries, even modest improvements in outcomes attributable to optimal systemic oxygenation strategies would have profound public health importance. Although the optimal approach to oxygenation in intensive care unit (ICU) patients with brain injuries remains uncertain, some recent data raise the possibility that the risks of harm arising from overzealous oxygen use in brain-injured patients may have been underestimated.
Hypoxic ischaemic encephalopathy
Concerns about the harms of liberal oxygen administration are particularly relevant in patients with hypoxic–ischaemic encephalopathy after cardiac arrest, where global ischaemia–reperfusion injury creates a substrate highly vulnerable to oxidative stress. Animal studies suggest that supraphysiological oxygen levels in the reperfusion phase exacerbate neuronal injury by promoting oxidative damage [2]. These mechanistic concerns underpin caution about the routine liberal use of oxygen in this setting.
The risk–benefit balance is especially nuanced in the immediate post-resuscitation period. While avoiding hypoxaemia remains a critical priority, liberal oxygen supplementation may expose patients to hyperoxaemia at precisely the time when the brain is most susceptible to reperfusion-related oxidative injury. Trials in the pre-hospital environment, such as the Reduction of Oxygen After Cardiac Arrest (EXACT) trial [3], highlight the difficulty of achieving precise oxygen targets in the pre-hospital setting. In the EXACT trial, a conservative strategy (SpO₂ 90–94% vs 98–100%) was associated with more frequent hypoxaemia episodes and a signal towards worse outcomes compared with usual care [3]. These findings suggest that, in the field, the dangers of under-oxygenation may outweigh those of transient hyperoxaemia. However, the findings of the EXACT trial are not generalizable to the ICU setting [3].
In the ICU, reliable monitoring with pulse oximetry and frequent arterial blood gases reduce the risk of inadvertent hypoxaemia, making conservative strategies more feasible. Subgroup analyses focussing on post-cardiac arrest patients in the ICU oxygen trials, Intensive Care Unit Randomized Trial Comparing Two Approaches to Oxygen Therapy (ICU-ROX) [4] and Pragmatic Investigation of Optimal Oxygen Targets (PILOT) [5], suggest potential mortality benefits with conservative oxygen therapy. By contrast, in Handling Oxygenation Targets in the ICU (HOT-ICU) [6], which enrolled only patients with hypoxaemic respiratory failure, no advantage of conservative therapy was seen in post-cardiac arrest patients, and point estimates favoured a liberal approach. Differences in patient selection and background hypoxaemia risk (regarding admission diagnosis and oxygen values at admission) may explain these discrepancies.
The largest and most rigorous study to date, the Blood Pressure and Oxygenation Targets in Postresuscitation Care (BOX) trial [7], found no significant difference in neurological outcomes or mortality between conservative and liberal oxygen targets in post-cardiac arrest patients; however, interpretation is complicated by limited separation in oxygen exposure between groups. Moreover, frequent early hyperoxaemia in the conservative oxygen arm, and overall outcomes that were better than typically observed in cardiac arrest cohorts, may have diluted potential signals of harm in patients allocated to liberal oxygenation.
The Low Oxygenation Goals in Cardiac Arrest Injury Limitation (LOGICAL) trial has completed recruitment of 1840 post-cardiac arrest patients who were randomly allocated to conservative or liberal oxygen [8]. The Mega randomised registry trial comparing oxygenation targets in adults in the intensive care unit with suspected hypoxic ischaemic encephalopathy (Mega-ROX HIE) [9], which will include approximately 4000 patients(< 12 h from injury), and targeting in patients allocated to conservative oxygen therapy the lowest possible FiO2 to achieve an SpO2 of ≥ 91% is also nearing completion. These trials should provide clinically meaningful data on whether concerns about liberal provision of oxygen in post-cardiac arrest patients in the ICU are justified.
Other acute brain injuries
Although inconsistently defined across studies, hyperoxaemia is consistently associated with mortality and poor neurological outcomes compared to normoxaemia in patients with intracerebral haemorrhage, ischaemic stroke, subarachnoid haemorrhage and traumatic brain injury [10]. Recent prospective observational data from traumatic brain injury (TBI) patients highlight that both high PaO₂ levels and large daily fluctuations in PaO₂ may be associated with high 6-month mortality and adverse neurological outcomes [11].
Recent data also highlight that, in patients with non-aneurysmal haemorrhage [12], hyperoxaemia (defined with different thresholds, PaO2 > 120–150 mmHg, > 300 mmHg) [13] is associated with unfavourable outcomes and with delayed cerebral ischaemia. These effects are mechanistically plausible because they may be a function of the cerebral vasoconstrictive effects of oxygen, which is often a physiological response to high PaO2 intended to protect the brain from oxidative stress, which then becomes maladaptive in the injured brain where autoregulation is already compromised.
ICU-specific randomised clinical trials (RCTs) evaluating oxygen strategies in stroke patients are not available. However, routine low-dose oxygen supplementation after stroke does not appear to affect death or disability rates at 3 months in non-hypoxaemia patients hospitalised with acute stroke [14]. A Chinese RCT in patients with anterior circulation ischaemic stroke who were candidates for endovascular treatment (normobaric hyperoxia treatment involved inhaling 100% oxygen at a flow rate of 10 L/min through a non-rebreather mask for 4 h, or an inspiratory oxygen fraction (FiO2) of 1 in participants for whom intubation was necessary. Sham treatment was 100% oxygen delivered at a flow rate of 1 L/min or an FiO2 of 0.3) showed that normobaric hyperoxaemia actually yielded superior functional outcomes at 90 days compared with control [15].
In the recently published UK-ROX trial [16], (which randomised patients all mechanically ventilated adults ICU patients to conservative oxygen therapy received the lowest fraction of inspired oxygen possible to maintain their Spo2 at 90%. vs oxygen therapy at the discretion of the treating clinician) day 90 mortality was 42.6% and 46.4% in non-HIE acute brain injury (no difference with HIE and non-HIE) patients allocated to conservative and usual oxygen therapy, respectively (risk difference -3.2 percentage points, 95% CI − 12.8 to 6.4 percentage points). Given the wide confidence intervals around treatment effect estimates, these data indicate that profoundly important effects on mortality attributable to oxygen regimens in brain-injured patients in the ICU have not been excluded.
The way forward
While hypoxaemia must be vigilantly avoided, accumulating data suggest that excessive oxygen exposure contributes to secondary brain injury. Observational studies consistently link hyperoxaemia with worse outcomes across multiple forms of acute brain injury, yet trial results remain mixed, often limited by challenges in separating treatment groups and heterogeneity of patient populations. Brain tissue oxygenation-directed therapies, such as PbtO₂ monitoring, may provide useful physiological insights but remain invasive, resource-intensive, and not widely applicable, and no level 1 evidence assessing its effect on outcome is available).
Large-scale, rigorously conducted RCTs nearing completion promise to clarify whether conservative systemic oxygen strategies can improve survival and neurological recovery compared with liberal approaches. Until such data are available, clinicians must balance the competing risks of hypoxaemia and hyperoxaemia, recognising that the optimal systemic oxygenation strategy in brain-injured ICU patients remains one of the most important unanswered questions in critical care. In addition, the definition of hyperoxia in terms of PaO₂, FiO₂ should be better clarified.
No comments:
Post a Comment