If your doctor can't predict and deliver 100% recovery, FIND SOMEONE COMPETENT!
Prediction of Stroke Outcomes in a Super-aged Society: Different Effects Among Predictive Variables
Published: March 02, 2026
DOI: 10.7759/cureus.104580 ![]()
Abstract
Background and objective: Population aging has progressed rapidly worldwide, particularly in developed countries such as Japan. Age is a well-established prognostic factor after stroke; however, its influence on functional outcomes may differ in increasingly older populations. This study aims to investigate whether the impact of age on post-stroke functional independence differs between patients aged ≥75 years (late elderly) and those aged <75 years.
Methods: This retrospective cohort study included 169 post-stroke patients admitted to a convalescent rehabilitation ward between 2018 and 2023. All patients were independent before stroke onset and received intensive multidisciplinary rehabilitation. Functional outcomes were assessed using the Functional Independence Measure (FIM), with the motor score at discharge as the primary endpoint. Patients were divided into a younger group referred to as the 'early elderly' (<75 years, n = 80) and an older group known as the 'late elderly' (≥75 years, n = 89). Multivariable linear regression analyses were performed for the entire cohort and separately for each age group, adjusting for demographic, clinical, and functional variables at admission.
Results: Baseline FIM motor and cognitive scores and trunk function were significantly poorer in the late elderly group; however, no significant age-related difference in FIM gain was observed. In the overall cohort, age, time from stroke onset to transfer, FIM cognitive score at admission, and trunk function independently predicted the FIM motor score at discharge. In subgroup analyses, age was not a significant predictor in the early elderly group but was a strong independent predictor in the late elderly group, along with cognitive function, motor impairment, trunk function, and time to rehabilitation.
Conclusions: The prognostic significance of age differs by age group in post-stroke rehabilitation. Age does not independently predict functional independence in patients aged <75 years, but plays a critical role among those aged ≥75 years. These findings highlight the need for age-specific prognostic models and rehabilitation planning in aging societies, particularly among patients undergoing intensive convalescent rehabilitation.
Introduction
Advances in public health and medical care have increased life expectancy worldwide, leading to rapid population aging. This demographic shift is particularly pronounced in developed countries. Japan is one of the most rapidly aging societies, with individuals aged ≥65 years accounting for more than 29% of the total population. In accordance with Japanese healthcare and social insurance policy, adults aged ≥65 years are classified as 'older,' those aged 65 to 74 years as 'early elderly,' and those aged ≥75 years as 'late elderly' [1]. This distinction reflects recognized differences in health status, functional reserve, and healthcare utilization between early and late elderly populations and provides a clinically meaningful framework for age-stratified analyses of functional outcomes.
Stroke is a leading cause of disability among older adults [2]. Residual hemiparesis and cognitive impairment are common after stroke and often result in substantial limitations in independence in activities of daily living (ADL) [3]. Early initiation of rehabilitation is essential for promoting functional recovery and independence [4]. Therefore, accurate prognostic prediction is critical for establishing appropriate rehabilitation strategies [5]. For example, when independent ambulation is unlikely, rehabilitation programs emphasize basic self-care activities such as eating, grooming, and dressing. In contrast, patients expected to regain ambulatory function may be assigned more advanced goals, including stair climbing. Numerous factors influence stroke outcomes, including initial stroke severity, lesion volume, and age, the latter of which has consistently been identified as a major determinant of prognosis [6].
However, the influence of age on stroke outcomes may differ from that reported in earlier studies, particularly in developed countries experiencing extreme population aging. Accordingly, this study investigated the impact of age on functional outcomes after stroke by comparing late elderly patients with their younger counterparts in a cohort from a rural region of Japan, where population aging is especially pronounced.
Materials & Methods
Study design and participants
This retrospective cohort study included post-stroke patients admitted to our convalescent rehabilitation ward between November 2018 and March 2023. During hospitalization, patients received up to 180 minutes per day of physical therapy, occupational therapy, and speech therapy, seven days per week, in accordance with the Japanese Guidelines for the Management of Stroke [7].
Eligibility criteria included a pre-stroke modified Rankin Scale (mRS) score of ≤2, indicating independence in ambulation and activities of daily living [8], and the absence of severe dementia. As in our previous studies [9-11], patients with subarachnoid hemorrhage or lesions involving the cerebellum or brainstem were excluded, as were those with medical complications requiring acute care (e.g., angina, gastrointestinal disease, or fractures). To minimize the influence of white matter lesions, only patients with a Fazekas score <2 were included [11,12]. The Fazekas scores were evaluated using MRI by an experienced physiatrist. The mRS was used solely as an eligibility criterion and is appropriately cited. No scale items, structured interview materials, or copyrighted content related to the mRS are reproduced in this manuscript.
Functional assessment
Functional status was assessed using the Functional Independence Measure (FIM) [13]. The FIM consists of 13 motor items and five cognitive items, each scored on a 7-point scale ranging from 1 (total assistance) to 7 (complete independence). Total scores range from 18 to 126, with motor subscale scores ranging from 13 to 91 and cognitive subscale scores from 5 to 35. Discharge was determined when the FIM motor score plateaued.
Functional improvement was quantified as FIM gain, defined as the change in the FIM motor score between admission and discharge, and was used as an indicator of rehabilitation effectiveness. The FIM was used solely for routine clinical scoring and outcome reporting. No copyrighted test forms, manuals, instructions, or item-level content are reproduced or described in this manuscript.
Assessment of motor and trunk function
Motor impairment was evaluated using the motor domain of the Stroke Impairment Assessment Set (SIAS), and trunk function was assessed using the SIAS trunk items [14]. Motor function for five components (upper limb, hand/fingers, hip, knee, and ankle) was scored on a 6-point scale (0-5). The sum of these components was calculated to assess the overall severity of motor impairment in the affected extremities (SIAS motor total).
Trunk function was scored from 0 to 6 based on vertical sitting balance and abdominal muscle strength (SIAS trunk), in accordance with the SIAS scoring system. The SIAS was used in accordance with standard academic practice; only summary scores were analyzed and reported, and no proprietary materials were reproduced.
Statistical analysis
Collected data included age, sex, type of stroke (ischemic (I) or hemorrhagic (H)), time from stroke onset to transfer, FIM and SIAS scores at admission and discharge, FIM gain, and total length of hospital stay (including the acute care period). The FIM motor score reflects functional performance [13], whereas SIAS scores assess neurological impairment [14]; therefore, these variables were considered complementary rather than redundant despite assessing related domains. Prior to age stratification, age was analyzed as a continuous variable in exploratory models to evaluate potential age-dependent changes in prognostic relationships.
Statistical analyses were performed in two steps. First, participants were divided into early elderly (<75 years) and late elderly (≥75 years) groups, and group differences were examined using Wilcoxon rank-sum tests or chi-squared tests, as appropriate. Continuous variables are presented as medians with interquartile ranges and were compared using the Wilcoxon rank-sum test due to non-normal distributions. Second, multiple linear regression analyses were conducted using the forced-entry method, with the FIM motor score at discharge as the dependent variable. Independent variables included age, type of stroke, time from onset to transfer, FIM motor and cognitive scores at admission, and SIAS motor total and SIAS trunk scores at admission.
Three regression models were constructed: one including all participants, one including only the early elderly group, and one including only the late elderly group. All statistical analyses were performed using the JMP software (SAS Institute Inc., Cary, NC, USA). A p-value <0.05 was considered statistically significant.
Results
Patient selection and baseline characteristics
The patient selection process is summarized in Figure 1. During the study period, 394 patients were admitted to the convalescent rehabilitation ward, of whom 169 met the eligibility criteria. Based on the predefined age cutoff of 75 years, 80 patients were assigned to the early elderly group and 89 to the late elderly group. Patient characteristics are presented in Table 1.
 Open Access
Open Access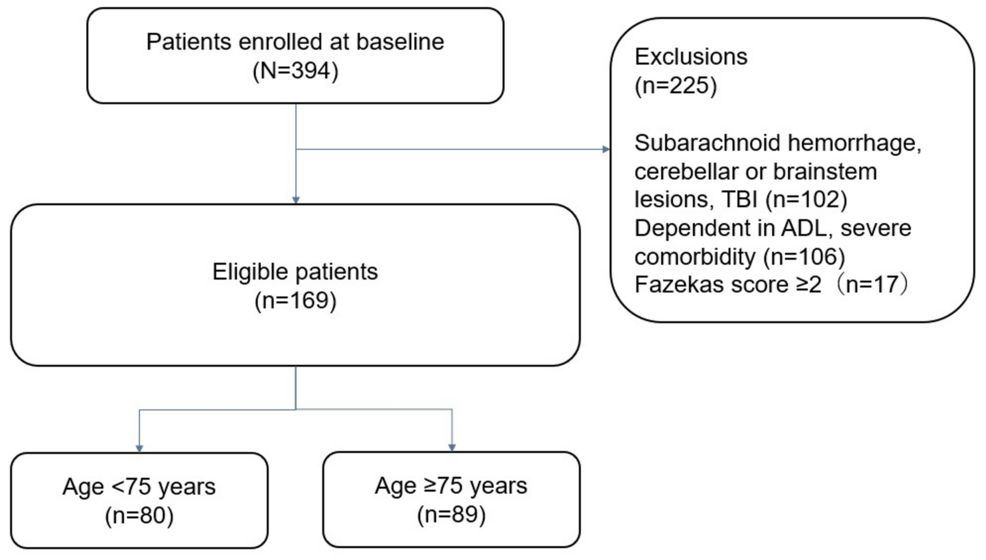
No comments:
Post a Comment